DESCRIPTION
DESCRIPTION
Background
What is Vitamin D?
In the liver, both vitamin D2 and D3 are metabolized into 25(OH)D, the inactive form of vitamin D. 25(OH)D is then converted into its activated form, 1,25(OH)2D in the kidneys. The biological role of 1,25(OH)2D is mediated through the vitamin D receptor (VDR). VDR binds to the retinoid X receptor (RXR) to form a heterodimer, which then binds to its ligand 1,25(OH)2D to form 1,25(OH)2D-VDR complex. The ligand-bound VDR complex then regulates gene expression by binding to the vitamin D response elements (VDRE), a sequence in the promoter region of the target gene (Hossein-Nezhad et al., 2014).
Vitamin D plays a pleiotropic role in the body. Research has shown that vitamin D regulates calcium metabolism, the immune system, cardiovascular system, and others. For instance, in the immune system, 1,25(OH)2D induces the expression of the gene CAMP, CD14, FN1, TREM1, which are responsible for encoding proteins involved in immediate response after infection (Saponaro et al., 2020).

Vitamin D Deficiency: A Global Pandemic
Announced by the NIH (National Institute of Health) as a global
pandemic, vitamin D deficiency (serum 25(OH)D level <50 nmol/L) has
already affected over 1 billion individuals around the world (Ibrahim,
et al 2020). Despite no obvious symptoms, around 50% of the global
population has vitamin D insufficiency issues (serum 25(OH)D level of
50 ~ <75nmol/L)(Holick et al, 2021; Amrein, et al, 2021; Charoenngam
et al., 2021).

Health professionals utilize serum 25(OH)D concentrations as the
marker for assessing vitamin D status instead of serum 1,25(OH)2D
concentrations since its supply is more plentiful in metabolites of
vitamin D in human serum. Furthermore, 25(OH)D is also more stable
compared to 1,25(OH)2D as it has a half-life of about 15 days while
1,25(OH)2D only has up to 15 hours, making 25(OH)D a better clinical
candidate for determination of vitamin D status(Thacher & Clarke,
2011). However, while it is most widely used for clinical
measurements, recent studies have suggested this method as unreliable
since it is 1,25(OH)2D that interacts with Vitamin D receptors(VDR)
and induces gene expression. Thus, the ratio of 1,25(OH)2D to 25(OH)D
(“Vitamin D activation ratio”) makes a much better indication for
determining vitamin D status in the human body (Thomas et al., 2020).
While there are several causes of deficiency, the most common reasons are the lack of exposure to sunlight and absorption of vitamin D from day-to-day diets (Holick, 2021). Without sufficient amounts of vitamin D, individuals start developing symptoms such as bone density loss, vulnerable immune system, and fatigue. Vitamin D deficiency also has strong associations to numerous chronic diseases, including bone metabolic disorders, tumors, and diabetes (Wang, et al 2017). In adults, vitamin D deficiency may worsen illnesses such as osteopenia, osteoporosis, and fractures. In children, lack of vitamin D can increase the chance of developing rickets, a rare bone disease that can cause bone pain, soft bones, and bone deformities (Vitamin D Deficiency, 2020; NHS Choices, 2018).
While there are several causes of deficiency, the most common reasons are the lack of exposure to sunlight and absorption of vitamin D from day-to-day diets (Holick, 2021). Without sufficient amounts of vitamin D, individuals start developing symptoms such as bone density loss, vulnerable immune system, and fatigue. Vitamin D deficiency also has strong associations to numerous chronic diseases, including bone metabolic disorders, tumors, and diabetes (Wang, et al 2017). In adults, vitamin D deficiency may worsen illnesses such as osteopenia, osteoporosis, and fractures. In children, lack of vitamin D can increase the chance of developing rickets, a rare bone disease that can cause bone pain, soft bones, and bone deformities (Vitamin D Deficiency, 2020; NHS Choices, 2018).
COVID-19 and Vitamin D
Known for regulating mineral metabolism, bone growth, and calcium
absorption, vitamin D shares several strong bonds with biological
actions during immunomodulation (Clarke, 2009). Recent studies even
suggest possible associations between the biological actions of
vitamin D and protection against COVID-19. This includes the
immunomodulatory effects of innate and adaptive immune systems,
reduction of viral entry in the kidney and lungs, as well as
protective effects against possible COVID-19 associated kidney
injuries (Charoenngam et al., 2021). Although vitamin D
supplementation’s potential in combating severity and intensity of
COVID-19 has not yet been confirmed, increasing amounts of scientific
experimentations support the claim. With COVID-19 on the roll,
increasing and maintaining vitamin D serum levels is without a doubt
beneficial in minimizing the damage caused by this disease
(Charoenngam et al., 2021).
Current Solutions and Problems
Supplements and Medication
One of the most common solutions to combat vitamin D deficiency is by
taking vitamin D supplements. For children, these supplements boost
bone growth and muscle density. For adults, it improves both bone and
mental health while combating prevalent issues like depression. This
form of treatment, however, is a short-term solution. Also, since
children often lack awareness towards the benefits of
supplements/medication, convincing them to take supplements
daily/regularly may prove to be a challenge in many households.
Furthermore, with amnesia caused by diseases such as Alzheimer's,
there is a high chance for adults/elders to forget to or over take
their medication/supplements. If patients do not take their pills
regularly, their serum 25(OH)D levels can easily drop below the normal
range (30 ng/mL,) (Tello, 2016). (NatureWise, 2021)

UV Light Therapy
Known as another alternative towards solving vitamin D deficiency, UVB
light therapy utilizes UVB rays to penetrate the skin in order to
increase conversion of 7-DHC into vitamin D3. During the treatment,
patients enter a room equipped with UVB lamps. UVB rays will then
initiate vitamin D metabolism, further increasing the patient's serum
vitamin D level. Despite this therapy’s advantage in combating vitamin
D deficiency, several dermatologists argue that at-home UVB light
treatment should not be implemented due to its perceived high risk,
including skin cancer, loss of skin elasticity, and eye problems.
Also, incorrect usage of UVB light lamps may induce gene damage and
mutation (Bhutani & Liao, 2010).

Theory
To create a better solution for combating vitamin D deficiency, we
engineer butyrate-producing bacteria.
Target Genes & Protein
Acetyl-CoA is the pathway that most butyrate-producing bacteria
species use to produce butyrate. As a result, it is the preferred
pathway for our project (Vital et al., 2014).

Gene in the Biological System
According to past research that assessed the butyrate metabolic
pathway by measurement of intracellular pathway intermediates in
recombinant Escherichia coli, the pool size measurement and
thermodynamic analysis showed the step converting Crotonyl-CoA to
butyryl-CoA as the rate-limiting step of the acetyl-CoA butyrate
synthesis pathway (Fischer et al., 2010). As a result, we identified
the bcd-etfAB gene, which encodes for butyryl-CoA dehydrogenase, as
our gene of interest.
The experiment also proves that the step converting acetoacetyl-CoA to (3S)-3-hydroxybutyryl-CoA is the rate-limiting step among the first three steps of the acetyl-CoA butyrate-producing pathway (from acetyl-CoA to Crotonyl-CoA) (Fischer et al., 2010). We, therefore, also target the hbd gene, which encodes for beta-hydroxybutyryl-CoA dehydrogenase.
The experiment also proves that the step converting acetoacetyl-CoA to (3S)-3-hydroxybutyryl-CoA is the rate-limiting step among the first three steps of the acetyl-CoA butyrate-producing pathway (from acetyl-CoA to Crotonyl-CoA) (Fischer et al., 2010). We, therefore, also target the hbd gene, which encodes for beta-hydroxybutyryl-CoA dehydrogenase.

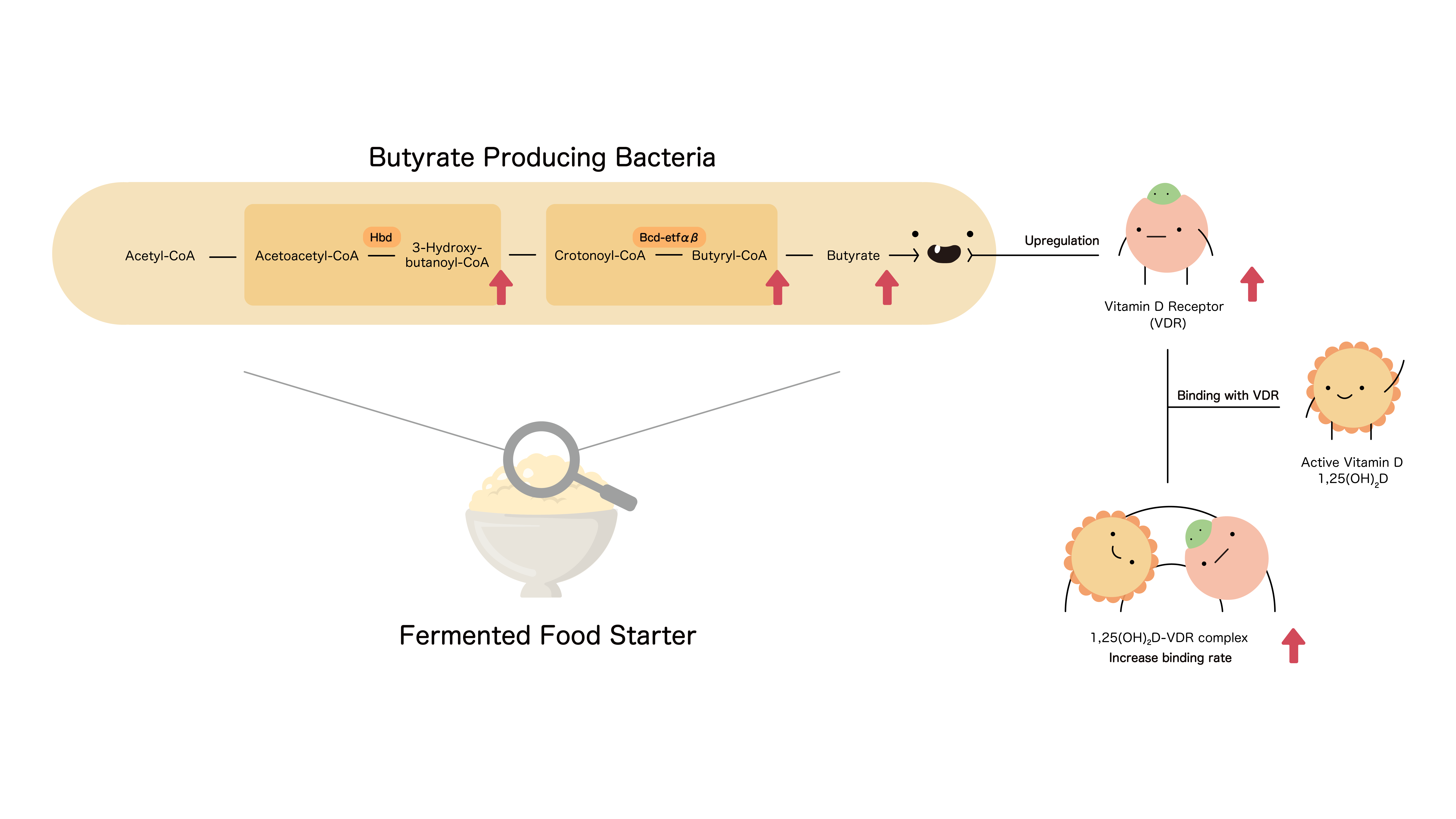
Our Solution
Butyrate is a short-chain fatty acid synthesized by probiotics in
human guts. It increases VDR (Vitamin D Receptor) expression in a time
and dose dependent manner through the activity of the TGFβ pathway
(Apprato, 2020).
Compared to the half-life of 25(OH)D (15 days), the half-life of the activated form, 1,25(OH)2D (15 hours) is relatively short. In the human body, 1,25(OH)2D is degraded and metabolized often before it is even utilized to exert downstream effects on certain genes, wasting activated vitamin D.
The upregulation of VDR increases the binding activity between VDR and the 1,25(OH)2D that would have been wasted otherwise. Increased binding activity will allow for the expression of certain health-related genes , thus helping the human body perform processes such as the regulation of the immune system and calcium homeostasis.
In order to create a better long-term solution to the problem of Vitamin D deficiency, we aim to enhance the butyrate-producing ability of probiotics.
To achieve our goal, we insert the target genes into the target probiotic. The hbd/ bcd-etfAB genes would result in the expression of beta-hydroxybutyryl-CoA dehydrogenase/ butyryl-CoA dehydrogenase, therefore increasing the rate of butyrate production.
Finally, we incorporate the resulting butyrate producing bacteria in the fermented food of countries worldwide to put our idea into practice.
Compared to the half-life of 25(OH)D (15 days), the half-life of the activated form, 1,25(OH)2D (15 hours) is relatively short. In the human body, 1,25(OH)2D is degraded and metabolized often before it is even utilized to exert downstream effects on certain genes, wasting activated vitamin D.
The upregulation of VDR increases the binding activity between VDR and the 1,25(OH)2D that would have been wasted otherwise. Increased binding activity will allow for the expression of certain health-related genes , thus helping the human body perform processes such as the regulation of the immune system and calcium homeostasis.
In order to create a better long-term solution to the problem of Vitamin D deficiency, we aim to enhance the butyrate-producing ability of probiotics.
To achieve our goal, we insert the target genes into the target probiotic. The hbd/ bcd-etfAB genes would result in the expression of beta-hydroxybutyryl-CoA dehydrogenase/ butyryl-CoA dehydrogenase, therefore increasing the rate of butyrate production.
Finally, we incorporate the resulting butyrate producing bacteria in the fermented food of countries worldwide to put our idea into practice.
Inspiration
When we first started as an iGEM team, our team started brainstorming
ideas about what kind of topics we would feel passionate about.
Looking at different research papers and recent studies about a wide
range of topics and taking inspiration from other iGEM teams, we found
a paper about “golden rice,” a genetically modified food. This Golden
rice project from 1999, although had several ethical oppositions,
still managed to help children in around 16 countries combat vitamin A
deficiency (Genetically Modified Organisms: The “Golden Rice” Debate).
Therefore, after deep consideration, our team also decided to dedicate
our project to something just as great, to help out others. And so, we
came up with the inspiration to do a project also related to vitamins,
which came to be vitamin D.
References
- Amrein, K., Scherkl, M., Hoffmann, M., Neuwersch-Sommeregger, S., Köstenberger, M., Berisha, A. T., Martucci, G., Pilz, S., & Malle, O. (2020, January 20). Vitamin D deficiency 2.0: an update on the current status worldwide. Nature News. https://www.nature.com/articles/s41430-020-0558-y.
- Apprato, G. (2020, June 14). Natural Epigenetic Modulators of Vitamin D Receptor.
- MDPI. https://www.mdpi.com/2076-3417/10/12/4096/htm Bhutani, T., & Liao, W. (2010). A Practical Approach to Home UVB Phototherapy for the Treatment of Generalized Psoriasis. Practical Dermatology, 7(2), 31–35. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4151182/
- Bordelon, P., Ghetu, M. V., & Langan, R. C. (2009). Recognition and Management of Vitamin D Deficiency. American Family Physician, 80(8), 841–846. https://www.aafp.org/afp/2009/1015/p841.htm
- Charoenngam, N., Shirvani, A., & Holick, M. (2021). Vitamin D and Its Potential Benefit for the COVID-19 Pandemic. Endocrine Practice, 27(5), 484–493. https://doi.org/10.1016/j.eprac.2021.03.006
- Collins, F. (2021). Office of Dietary Supplements - Vitamin D. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/.
- Clarke, B. (2009). Vitamin D - an overview | ScienceDirect Topics. Www.sciencedirect.com. https://www.sciencedirect.com/topics/pharmacology-toxicology-and-pharmaceutical-science/vitamin-d
- Demmer, J. K., Pal Chowdhury, N., Selmer, T., Ermler, U., & Buckel, W. (2017). The semiquinone swing in the bifurcating electron transferring flavoprotein/butyryl-CoA dehydrogenase complex from Clostridium difficile. Nature Communications, 8(1). https://doi.org/10.1038/s41467-017-01746-3
- “Ergocalciferol (Vitamin D2) Oral: Uses, Side Effects, Interactions, Pictures, Warnings & Dosing - WebMD.” Webmd.com, 2021, www.webmd.com/drugs/2/drug-8604/ergocalciferol-vitamin-d2-oral/details#:~:text=Vitamin%20D%20ergocalciferol%2DD2%2C,building%20and%20keeping%20strong%20bones..
- Fischer, C. R., Tseng, H. C., Tai, M., Prather, K. L. J., & Stephanopoulos, G. (2010). Assessment of heterologous butyrate and butanol pathway activity by measurement of intracellular pathway intermediates in recombinant Escherichia coli. Applied Microbiology and Biotechnology, 88(1), 265–275. https://doi.org/10.1007/s00253-010-2749-2
-
Holick, M. F., & Chen, T. C. (2021). Vitamin D deficiency: a
worldwide problem with health consequences. The American journal of
clinical nutrition.
https://pubmed.ncbi.nlm.nih.gov/18400738/#:~:text=Vitamin%20D%20deficiency%20has%20been,Ds
%20beneficial%20effects%20for%20health. - Holick MF. (2014). Sunlight, ultraviolet radiation, vitamin D and skin cancer: how much sunlight do we need? Advances in Experimental Medicine and Biology, 810. https://doi.org/
- Hossein-Nezhad, A., Eshaghi, S. M., Maghbooli, Z., Mirzaei, K., Shirzad, M., Curletto, B., & Chen, T. C. (2014, March 6). The Role of Vitamin D Deficiency and Vitamin D Receptor Genotypes on the Degree of Collateralization in Patients with Suspected Coronary Artery Disease. BioMed Research International. https://www.hindawi.com/journals/bmri/2014/304250/
-
Ibrahim, M. K. M., & Elnimeiri, M. K. M. (2020, August 10).
Non-classical presentation of vitamin D deficiency: a case report.
Journal of Medical Case Reports.
https://jmedicalcasereports.biomedcentral.com/articles/10.1186/s13256-020-02454-1#:~:text=About%20one%20billion%20people%20globally,home%20residents%2C%20and%20
hospitalized%20patients. - INTERACTIVE MAPS ON VITAMIN D LEVEL WORLDWIDE. (2012). https://revista-fi.com.br/upload_arquivos/201606/2016060819177001467124549.pdf
- Nair, R., & Maseeh, A. (2012, April). Vitamin D: The "sunshine" vitamin. Journal of pharmacology & pharmacotherapeutics. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3356951/.
- NatureWise. (2021). NatureWise. https://www.naturewise.com/products/vitamin-d3-2-000-iu-subscription
- NHS Choices. (2018, May 25). Overview - Rickets and osteomalacia. NHS. https://www.nhs.uk/conditions/rickets-and-osteomalacia/
- Office of Dietary Supplements - Vitamin D. (2017). Nih.gov. https://ods.od.nih.gov/factsheets/VitaminD-Consumer/
- Phototherapy | UV Light Therapy - Toronto Dermatology Centre. (2021). Https://Torontodermatologycentre.com/. https://torontodermatologycentre.com/phototherapy/
- Pros and Cons of Vitamin Supplements. (2013). Explorevitamins.co.uk. http://www.explorevitamins.co.uk/Pros-and-Cons-of-vitamin-supplements.html
- Pros and Cons of UVC LEDs and Lamps for Disinfecting Applications. (2020). Ledinside.com. https://www.ledinside.com/news/2020/8/uvc_light_comparison
- Saponaro, F., Saba, A., & Zucchi, R. (2020). An Update on Vitamin D Metabolism. International Journal of Molecular Sciences, 21(18). https://doi.org/10.3390/ijms21186573
- Tello, M. (2016, December 19). Vitamin D: What’s the. Harvard Health; Harvard Health. https://www.health.harvard.edu/blog/vitamin-d-whats-right-level-2016121910893
- Thacher, T. D., & Clarke, B. L. (2011). Vitamin D Insufficiency. Mayo Clinic Proceedings, 86(1), 50–60. https://doi.org/10.4065/mcp.2010.0567
- Thomas, R. L., Jiang, L., Adams, J. S., Xu, Z. Z., Shen, J., Janssen, S., Ackermann, G., Vanderschueren, D., Pauwels, S., Knight, R., Orwoll, E. S., & Kado, D. M. (2020). Vitamin D metabolites and the gut microbiome in older men. Nature Communications, 11(1), 5997. https://doi.org/10.1038/s41467-020-19793-8
-
U.S. National Library of Medicine. (2020, June 12). Vitamin D
Deficiency. MedlinePlus.
https://medlineplus.gov/vitaminddeficiency.html#:~:text=Vitamin%20D%20deficiency%20can%20lead,to%20become
%20soft%20and%20bend. - Vital, M., Howe, A. C., & Tiedje, J. M. (2014). Revealing the Bacterial Butyrate Synthesis Pathways by Analyzing (Meta)genomic Data. MBio, 5(2). https://doi.org/10.1128/mbio.00889-14
- Vitamin D: Pros and Cons - MedShadow. (2019, July 21). MedShaow. https://medshadow.org/vitamin-d-pros-cons/
- Vitamin D toxicity: What if you get too much? (2020). Mayo Clinic; https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/expert-answers/vitamin-d-toxicity/faq-20058108#:~:text=The%20main%20consequence%20of%20vitamin,the%20formation%20of%20calcium%20stones.
- Wacker, M., & Holick, M. F. (2013). Sunlight and Vitamin D. Dermato-Endocrinology, 5(1), 51–108. https://doi.org/10.4161/derm.24494

